Revolutionizing Drug Delivery
Drug delivery to cancer cells with minimum side effect has long been a big challenge in cancer treatment. Using L-glucose as a drug delivery system, we make a breakthrough in the fight against refractory cancers.
The drug delivery can be analogous to the “Trojan horse”(*1) strategy that the ancient Greeks used to hide their armed troops to invade the Trojan army in the Trojan War. The “horse” molecule that leads the “weapon” molecule enters cancer cell (Figure 1) . The “horse” molecule and the “weapon” molecule are connected by a strong chemical bond that cannot be easily broken.

【Figure 1】 The “Trojan Horse” strategy in cancer treatment.
What is the ORBIO method for cancer treatment?
The ORBIO method uses L-glucose as the “horse” in the “Trojan Horse” strategy. The “horse” carries functional molecules being conjugated by a strong chemical bond. The functional molecules are taken up by cancer cells with an unprecedented high selectivity. The cancer cells are then destroyed by the toxicity of the functional molecules themselves, or by further activating the functional molecules physically.
D-glucose (right in Figure 2) is the most fundamental nutrient and energy source for nearly all cells. On the contrary, its mirror-image isomer, L-glucose (left in Figure 2) occurs rarely in nature. Even if it were synthesized and provided, mammalian cells do not take it up as a nutrient. Beyond expectations, Dr. Katsuya Yamada (currently the specially-appointed professor at ORBIO Joint Research Laboratory, Hirosaki University) and his colleagues have discovered that cancer cells take in L-glucose bearing a green fluorescent group called NBD as if it were a nutrient. When they changed the fluorescent group to a blue 7-OH-coumarin, cancer cells not only took it up, but also captured into their nuclei. 7-OH-coumarin, also known as umbelliferone, has been shown to exhibit anti-tumor effects against various cancer cells (Akkol E.K. et al., Cancers 12: 1959, 2020; Zhang L. et al., Eur. J. Med. Chem. 2019). L-glucose derivatives bearing these fluorescent groups were selectively taken up by various cancer cells including refractory adenocarcinomas such as pancreatic, biliary tract, and ovarian cancers, as well as in sarcomas. Then, a completely new modality that captures the dynamics of cancer cells has been proposed in cancer diagnosis. Based on these discoveries, ORBIO Corporation is developing novel techniques that will make the drug delivery system in oncotherapy a step forward. In our approach, L-glucose is used as the “horse” molecule in a “Trojan Horse” strategy. A series of new molecules which combine L-glucose with functional “weapons” are referred to as ORBIO molecules. Use of L-glucose as the “horse” assures unprecedentedly high preference for cancer cells. An adequate design of the functional “weapon” enables cancer cells to take in L-glucose, the “horse”, with the “weapon” molecules. Further activating the “weapon” molecules using physical methods is possible depending on the molecular types attached to facilitate the cancer cell death.
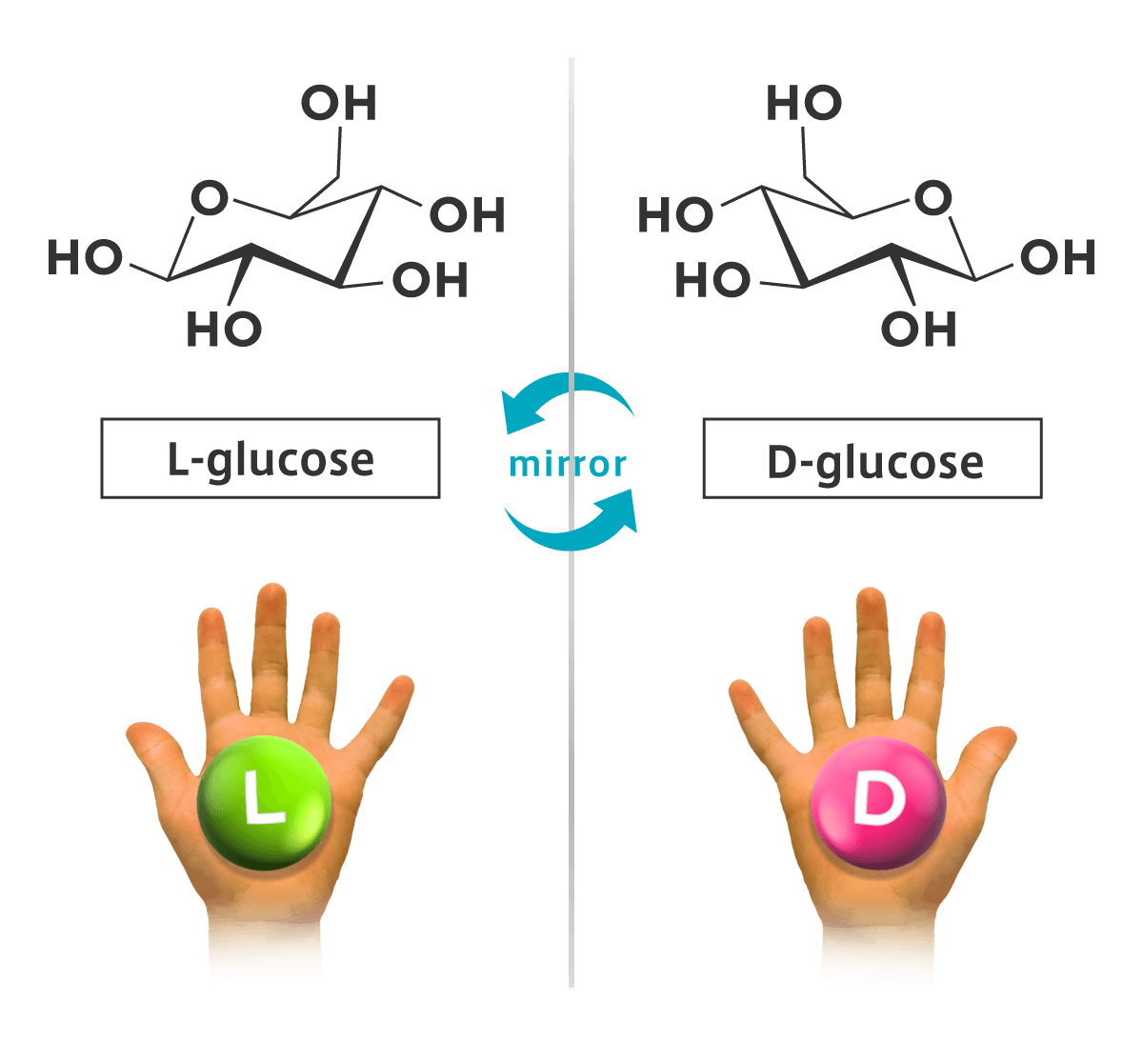
【Figure 2】 Chemical structures of D-glucose (right) and L-glucose (left). The structures are mirror images of each other.
The principal feature of the cancer conquest method using the ORBIO molecule, or the “ORBIO method”, is its extremely high cancer specificity: L-glucose is least to be taken up by normal cells. We have successfully completed an expanded single-dose toxicity test and a mutagenicity test at a good laboratory practice (GLP) examination for two of fluorescente L-glucose. All adenocarcinoma cells so far tested take in the L-glucose derivative. These include cells in refractory cancers such as cancers in pancreas and biliary tract, osteosarcoma, and ovarian, uterine, and gastric cancer with poor prognosis. As shown in Figure 3, we have reported that this uptake is mediated by a channel-like protein (*3) (Sasaki, A. et al., Human Cell 29: 37-45, 2016), which is specifically expressed in cancer cells.
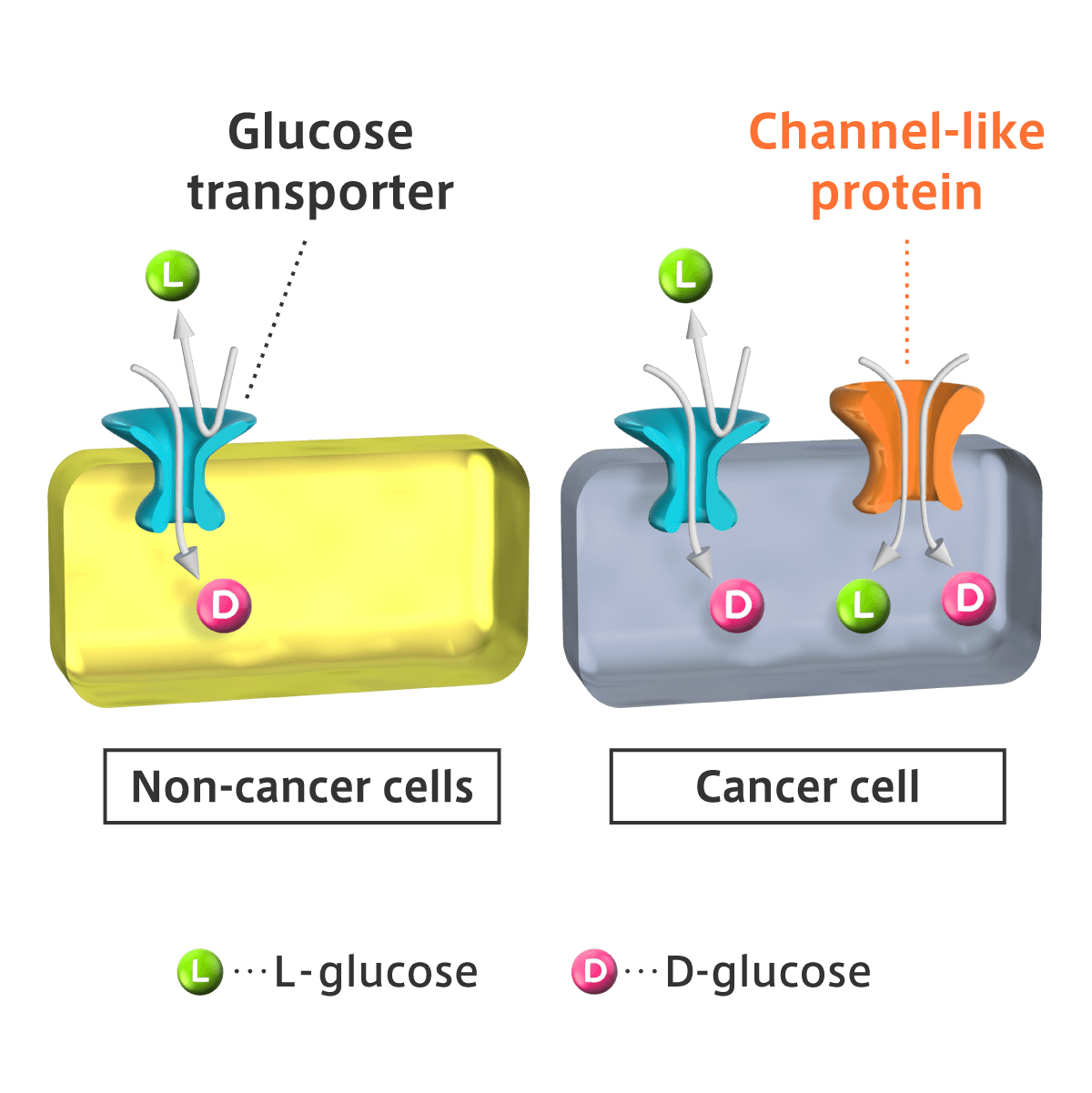
【Figure 3】 Specific uptake of L-glucose into cancer cells. Here, glucose transporter(*2) attracts only D-glucose into the cell.
The second feature of the “ORBIO Method” is its potential to start cancer treatment in very early stages. Unlike conventional surgery, which attempts to remove cancers as they grow at the macroscopic level, the “Trojan Horse” works microscopically. Even in stages when only a few cancer cells can be detected, barely detectable by the latest diagnostic methods such as PET, CT, US, and MRI, the “ORBIO Method” has a potential to detect them and achieve earliest possible control of the progression of cancer. Furthermore, even when cancers are detected too late to be resected at Stage 4, or where metastases are too small to be detected by usual imaging modalities such as PET, the “weapon” molecules are able to be selectively delivered to cancer cells with minimum adverse side effects. Figure 4 represents symbolically that tumor cells exhibiting malignant features selectively take up L-glucose bearing a green fluorescent group and emit green fluorescence among cells derived from the pancreas.
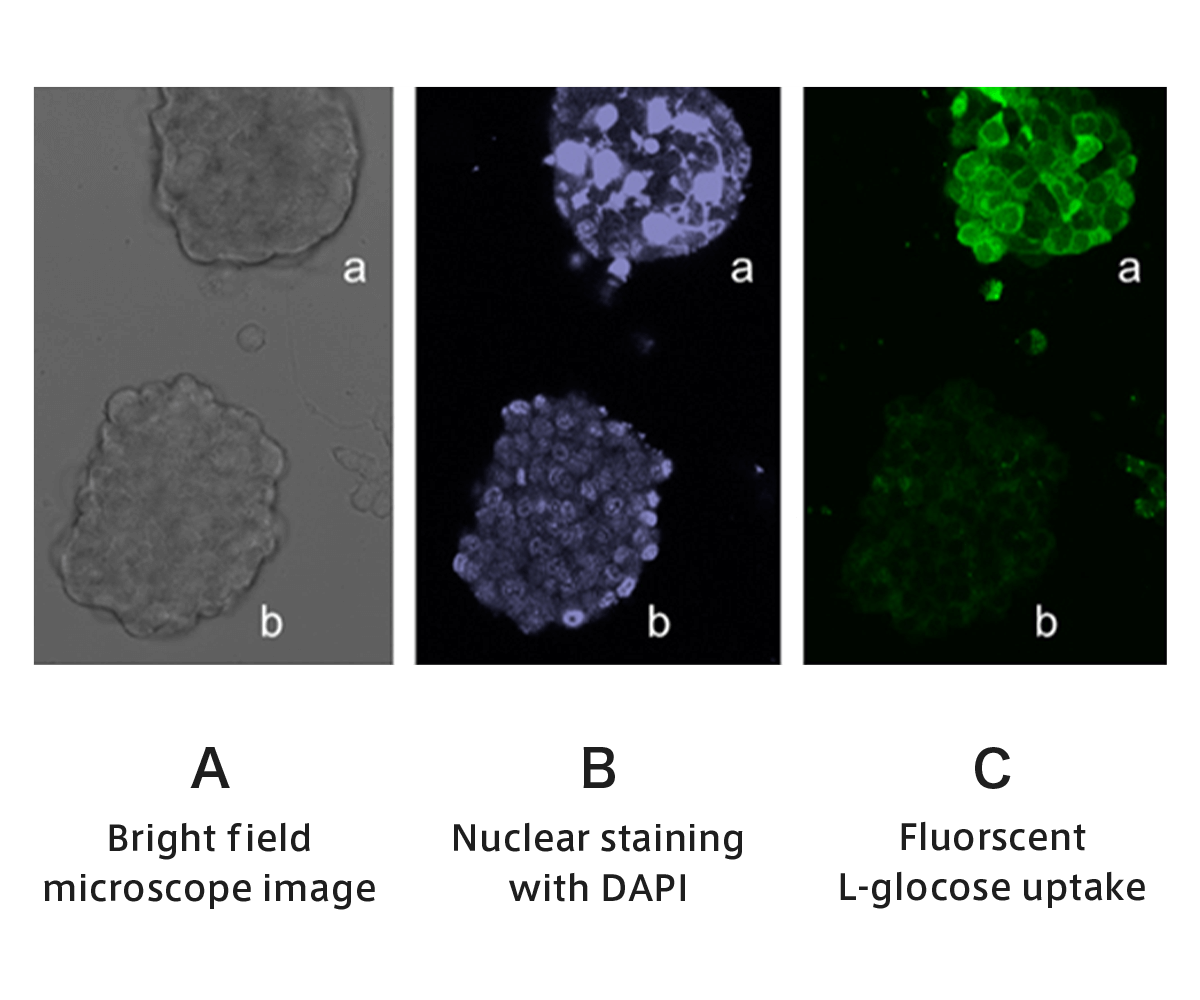
【Figure 4】 Of the tumor cell masses a and b derived from a mouse pancreas (A), only a, which is a malignant tumor exhibiting nuclear atypia characteristics (B), strongly uptakes fluorescent L-glucose into the cells (C). In contrast, mass b, which exhibits the nuclear characteristics of a benign tumor or normal cell (B), does not uptake fluorescent L-glucose (C).
Anticancer Drug Candidates-1: CLG
As the first molecule to realize the ORBIO method, we propose a novel compound, named CLG. CLG consists of L-glucose, which is selectively taken up by cancer cells as the “horse” molecule, and 7-OH-Coumarin, which emits blue fluorescence and is found widely in such as carrots, parsley, and mandarin oranges, as the “weapon” molecule. We confirmed that CLG enters cancer cells, then into their nuclei, eventually inhibits their growth.
The molecular structure of CLG is shown in Figure 5. CLG is an L-glucose derivative attaching 7-OH coumarin tightly to the carbon-2 position via a nitrogen linker. After entering cancer cells, CLG emits blue fluorescence due to its coumarin moiety, further enters the nucleus of cancer cells, and impairs their proliferation. Using pancreatic tumor cells, we repeatedly confirmed that CLG suppress the tumor cell proliferation in a dose-, and time-dependent manner. Collapsing cell masses were detected by a longer exposure to CLG. In our preliminary experiments, a concentration of CLG at least over 250 mg/kg (i.p. mice) can be safely administered in vivo, encouraging further development of CLG to pre-clinical/clinical stages.
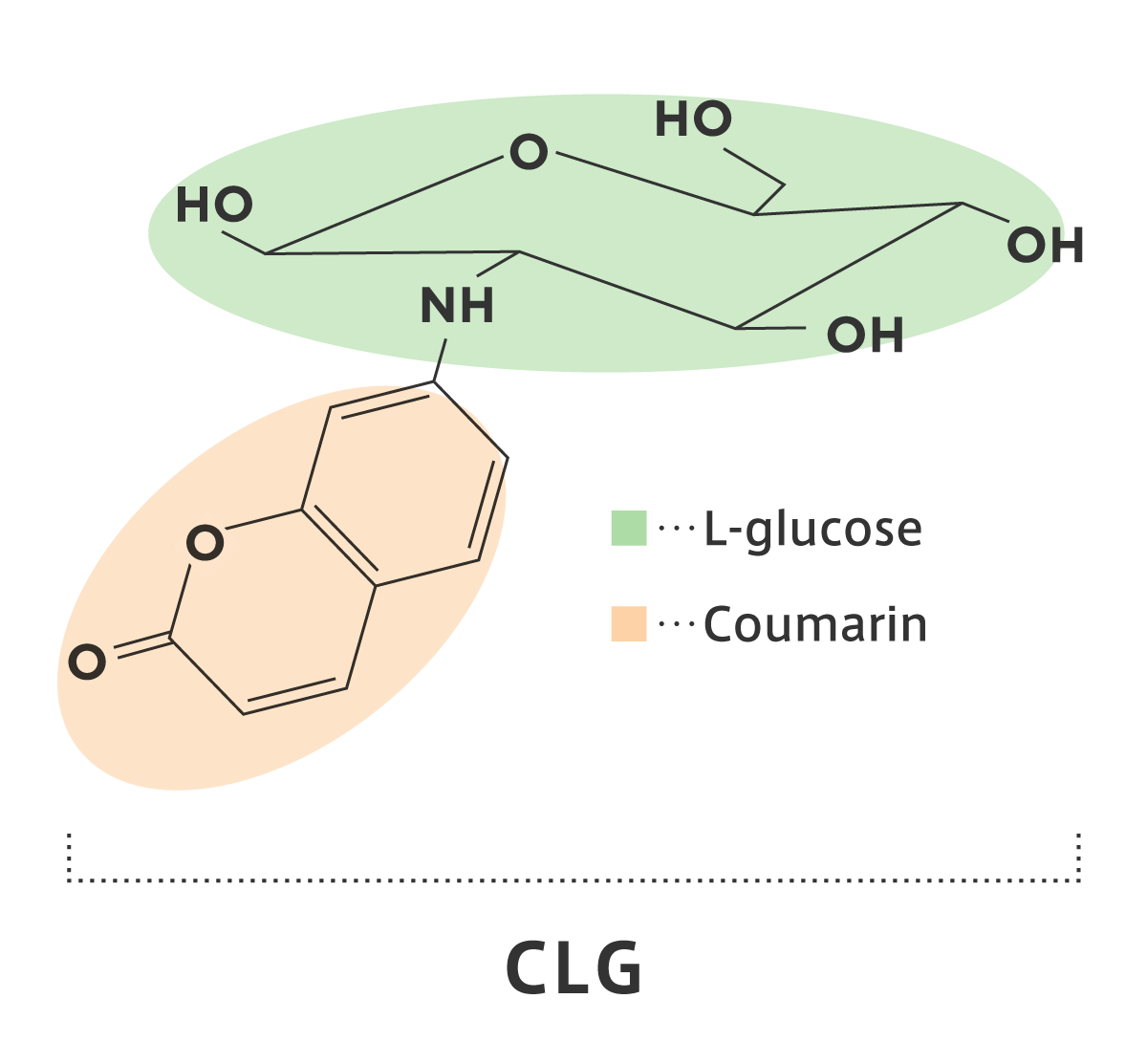
【Figure 5】 Molecular structure of CLG bearing a coumarin group (7-OH-coumarin), which is tightly bound to the L-glucose via a nitrogen linker.
New Anticancer Drug Candidates-2: ALG
As the second molecule to embody the ORBIO method, we created a new substance that uses L-glucose, which is selectively taken up by cancer cells, as the “horse” molecule and an organic compound of gold (Au) as the “weapon” molecule, which we named ALG. We then discovered that ALG causes cell death. Therefore, it is expected to be a promising candidate as an anticancer drug.
Focusing on the selectivity of cancer cells to specifically take up L-glucose intracellularly, we created a new substance by sulfide bonding an organic group Au-P- (C2H5) 3 with gold (Au) to L-glucose and named it ALG (Figure 6). After ALG was taken up into the cell, we discovered that the organic Au group was toxic. Therefore, ALG is also expected to be an anticancer drug with extremely strong cancer cell selectivity. Furthermore, since gold (Au) accumulates in cancer cells, after administering ALG, high-frequency radio waves are scanned from outside the body. Then, only cancer cells in which Au has accumulated are expected to generate heat by high frequency radio wave. In this way, only cancer cells are heated and exposed to higher temperatures and normal cells can be kept at lower temperatures, which is expected to ensure the death of cancer cells (high-frequency hyperthermia therapy).
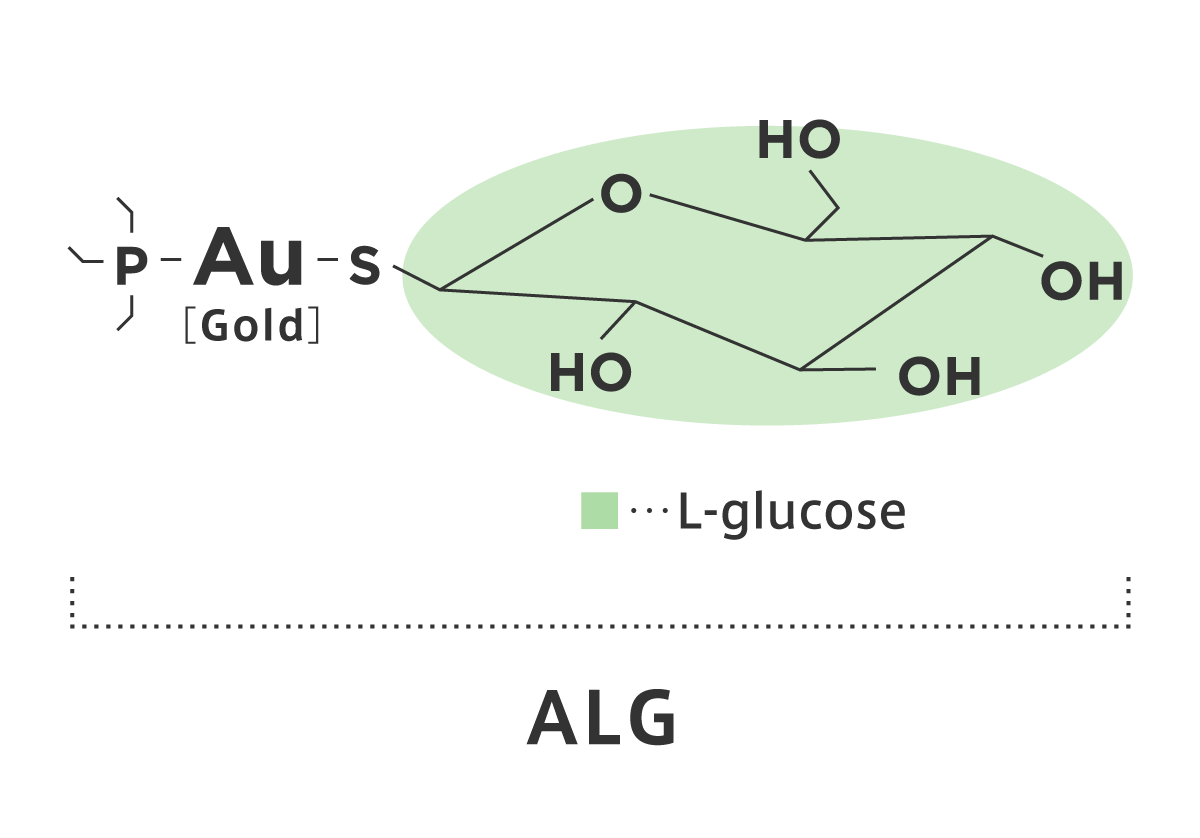
【Figure 6】 Molecular structure of ALG, in which an organic Au group is tightly attached to L-glucose via a sulfide bond.
What is the difference from conventional anti-cancer drugs?
In contrast to conventional anti-cancer drugs that attack both cancer cells and normal cells, or that act on specific molecules expressed in a subset of cancers, the ORBIO molecules use unusual nutrients, i. e., L-glucose as “Trojan Horse” that only cancer cells can utilize.
Conventional anti-cancer drugs indiscriminately attack both cancer cells and normal cells that proliferate actively to suppress the local growth of and metastasis of cancer cells, resulting in serious side effects on normal cells. In other words, the dose amount of anti-cancer drugs that produces favorable effects, and the dose amount that produces adverse effects are usually very close in conventional anticancer drugs; however, the dose amount at which side effects appear in ORBIO method is likely to be considerably higher than the dose amount that produces anticancer effects and it can be expected that ORBIO method will cause few or no side effects. Recent "molecular targeted drugs" are designed to act on molecules expressed relatively more in a specific subset of cancers. This feature would critically limit the cancer types they work on. However, these "molecular targeted drugs" can more or less impair normal cells as well and sometimes cause unpredictable side effects. In contrast to these strategies targeting molecules, usually proteins, expressing "specifically" on cancer cells, the design concept of ORBIO molecules is an approach to use unusual nutrients “L-glucose” that only abnormal cells can utilize regardless of protein types to take them in.
